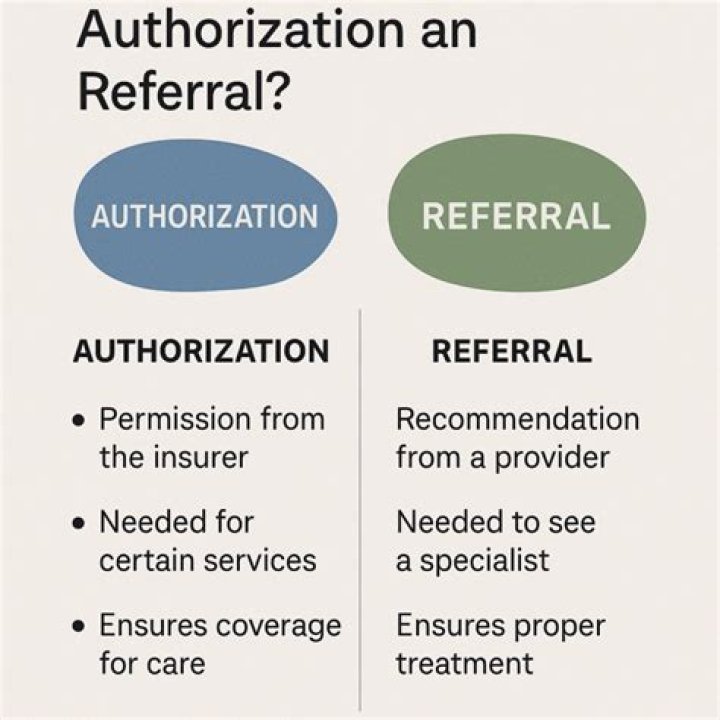
Are referrals required for Humana
For all other beneficiaries enrolled in a TRICARE Prime plan, your PCM gives you a referral for most services that he or she can’t provide. If you have TRICARE Select, referrals are not required, but you may need prior authorization from Humana Military for some services.
Does Humana PPO require referrals?
Unlike an HMO, a PPO offers you the freedom to receive care from any provider—in or out of your network. This means you can see any doctor or specialist, or use any hospital. In addition, PPO plans do not require you to choose a primary care physician (PCP) and do not require referrals.
Do Humana HMO plans require referrals?
Do I have to use a primary care physician (PCP)? With most HMO plans, all of your healthcare services are coordinated by your designated PCP. PPO plans do not require referrals for any services.
How do I get a referral for Humana?
800-266-3022. For same-day appointments or urgent requests, call 800-523-0023. To create a new referral or authorization online, visit Availity.com, which is available 24/7 for your convenience. This form does not guarantee payment by Humana Inc.What does Humana pay for?
Original Medicare Part B – medical coverage Medically necessary doctors’ services. Outpatient care. Medically necessary chiropractic care. Home health services.
Do doctors prefer PPO or HMO?
A PPO plan can be a better choice compared with an HMO if you need flexibility in which health care providers you see. More flexibility to use providers both in-network and out-of-network. You can usually visit specialists without a referral, including out-of-network specialists.
How do I check my Humana authorization?
- Electronic requests: CoverMyMeds® is a free service that allows prescribers to submit and check the status of prior authorization requests electronically for any Humana plan. …
- Phone requests: Call 1-800-555-CLIN (2546), Monday – Friday, 8 a.m. – 8 p.m., local time.
Which pays better HMO or PPO?
In general, HMO premiums are lower than other plans (like PPOs) that give you more flexibility. Additionally, you may pay less for deductibles, copays, and prescriptions with HMOs. PPO premiums are higher than HMOs. You also typically pay more for out-of-pocket costs like deductibles and copays.What's the difference in a HMO and a PPO?
What Is the Difference Between an HMO and a PPO? … With an HMO plan, you must stay within your network of providers to receive coverage. Under a PPO plan, patients still have a network of providers, but they aren’t restricted to seeing just those physicians. You have the freedom to visit any healthcare provider you wish.
Does Humana cover hysterectomy?Humana – CareSource covers abortions, hysterectomy and sterilizations in very limited circumstances. … Visit the “Forms” section of our website for all appropriate forms to complete for an abortion, hysterectomy or sterilization.
Article first time published onDoes Humana cover sleep studies?
Yes, Humana covers and accepts a variety of home sleep tests.
Does Humana cover skin removal surgery?
Humana Medicare Advantage plans can cover dermatology services that are medically necessary, such as treatments for psoriasis, eczema and more, though they typically don’t cover cosmetic dermatology.
What does Humana HMO mean?
HMO stands for health maintenance organization. HMOs have their own network of doctors, hospitals and other healthcare providers who have agreed to accept payment at a certain level for any services they provide.
Is Humana Dental PPO or HMO?
Humana’s affordable PPO Preventive Plus dental insurance plan covers your and your family’s preventive care and basic services. This PPO plan does not require you to choose a primary care dentist. Instead, you can choose any dentist in or out of network, though your costs will be higher with out-of-network dentists.
Is Humana gold the same as Medicare?
Humana Gold Plus HMO plans offer affordable or even $0 monthly premiums, coverage that provides more benefits than Original Medicare and the security of a maximum annual out-of-pocket cost. Nearly 60% of all Medicare Advantage plan members choose an HMO plan for their coverage.
Does Humana have an out of pocket maximum?
Out-of-pocket maximum With most Humana plans, there is a maximum amount that you’ll be required to pay out-of-pocket. Deductibles and copayment go toward this out-of-pocket maximum. Once the total amount you’ve paid reaches the out-of-pocket maximum, your plan pays 100 percent of covered services.
How long does it take to get hired at Humana?
The hiring process is about 2 weeks. There was a 2 second interview. If they are interested in you it moves pretty quickly, HR calls and sets thing’s up fast.
Can you have Medicare and Humana at the same time?
No Medicare and Humana are not the same. Humana is one of the largest private insurance companies that provides, along with other products, Medicare Advantage plans and Medicare Part D prescription drug plans.
Does Medicare require authorization in 2021?
Effective January 1, 2021, prior authorization will be required for certain services on the Medicare Prior Authorization List. This link can also be found on Superior’s Prior Authorization and Superior’s Provider Forms webpages. … Prior authorization is subject to covered benefit review and is not a guarantee of payment.
How do I submit a prior authorization to Humana?
- Submit an online request for Part D prior authorization.
- Download, fill out and fax one of the following forms to 877-486-2621: Request for Medicare Prescription Drug Coverage Determination – English. …
- Call 800-555-CLIN (2546), Monday – Friday, 8 a.m. – 8 p.m., local time.
Does Humana cover blood transfusions?
Plan A covers your Medicare Part A coinsurance, Part B coinsurance/copayments, the first three pints of blood needed for a transfusion and hospice care copayments and coinsurance.
What is FFS insurance mean?
Fee-for-Service (FFS) Plans (non-PPO) A traditional type of insurance in which the health plan will either pay the medical provider directly or reimburse you after you have filed an insurance claim for each covered medical expense. When you need medical attention, you visit the doctor or hospital of your choice.
Is EPO and PPO the same?
A PPO offers more flexibility with limited coverage or reimbursement for out-of-network providers. An EPO is more restrictive, with less coverage or reimbursement for out-of-network providers. For budget-friendly members, the cost of an EPO is typically lower than a PPO.
Is Blue Shield Good?
Blue Shield of California earned a Top 5 rating in our annual review of Best Health Insurance Companies. They got 4 out of 5 star ratings across the board in claims, price and customer service and 4-star ratings in website & apps.
Is it better to have a high or low deductible for health insurance?
Key takeaways. Low deductibles are best when an illness or injury requires extensive medical care. High-deductible plans offer more manageable premiums and access to HSAs. HSAs offer a trio of tax benefits and can be a source of retirement income.
How do I find out my deductible?
A deductible can be either a specific dollar amount or a percentage of the total amount of insurance on a policy. The amount is established by the terms of your coverage and can be found on the declarations (or front) page of standard homeowners and auto insurance policies.
Are HMOs bad?
Explaining HMOs Since HMOs only contract with a certain number of doctors and hospitals in any one particular area, and insurers won’t pay for healthcare received at out-of-network providers, the biggest disadvantages of HMOs are fewer choices and potentially, higher costs.
Does PPO have copay?
Because PPO plans don’t require a PCP, they offer more convenience but can also be more expensive. If you choose a copay PPO plan, you will have to pay a copay (a fixed dollar amount) each time you visit a provider. Generally, a PPO plan with a copay has lower premiums than a comparable non-copay plan.
Why is PPO more expensive?
PPO plans generally are more expensive than HMO plans. However, due to the pooling of people in a PPO network, fees associated with health care will be lower for participants. In other words, you will pay far less for services if you are in a PPO plan vs. not having insurance at all.
In which of the following plans will your insurance not pay if you go out-of-network?
Some health plans, such as an HMO plan, will not cover care from out-of-network providers at all, except in an emergency.
Is Humana a good company?
Not only one of the biggest Medicare plans, Humana is one of the highest-rated overall. Not all their subsidiaries score as well for quality or customer satisfaction, so verifying the ratings of your specific options is important. They also offer a range of ways to sign up and interact with the plan.